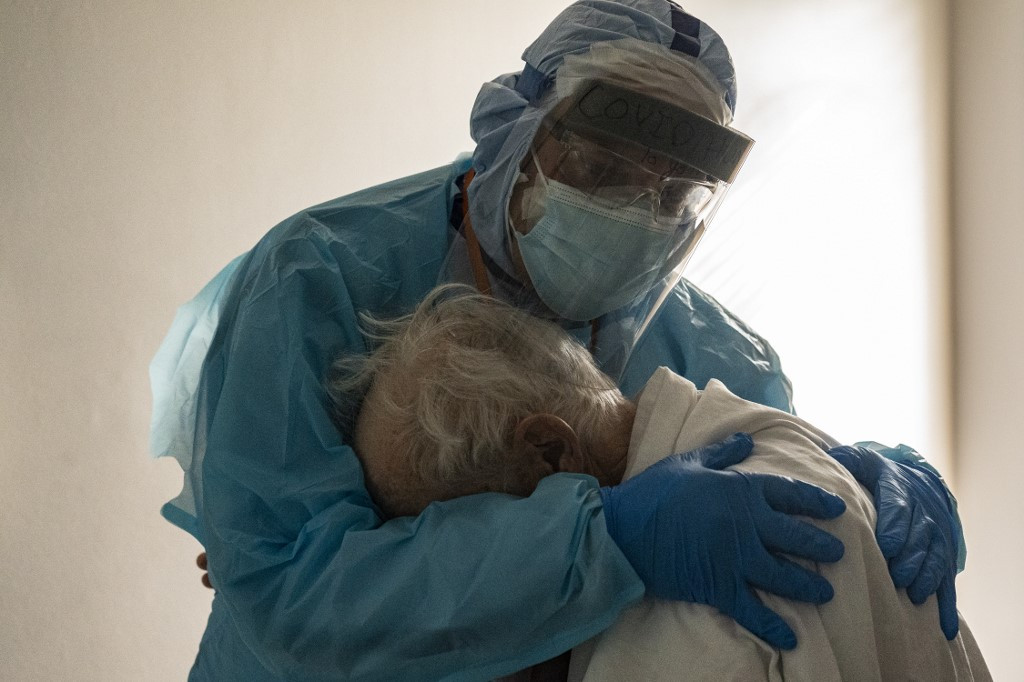
As a stubborn third wave of COVID-19 rages through the country, exhausted doctors, nurses, and other health sector workers have a solitary plea to the public: “please think of one another, rather than just yourself.”
“Work is tiring and exhausting,” one doctor told Roar Media. “It keeps getting worse. They [hospital administration] just keep adding beds and beds and beds without having any sense of how they are going to allocate staff. As a result, one or two doctors have to take care of 150-200 patients. You get fed up, naturally.”
Doctors in Sri Lanka are now logging up to 240-340 work hours a month. A single shift can last a minimum of 24 hours. And if one is assigned to a COVID-19 intermediate care centre, then chances are work hours will be even more.
We recently spoke to three local doctors battling the pandemic from the frontlines: one works at a COVID-19 intermediate care centre, one is a surgeon at a base hospital, and the third works at a neonatal ward. All three doctors requested anonymity.
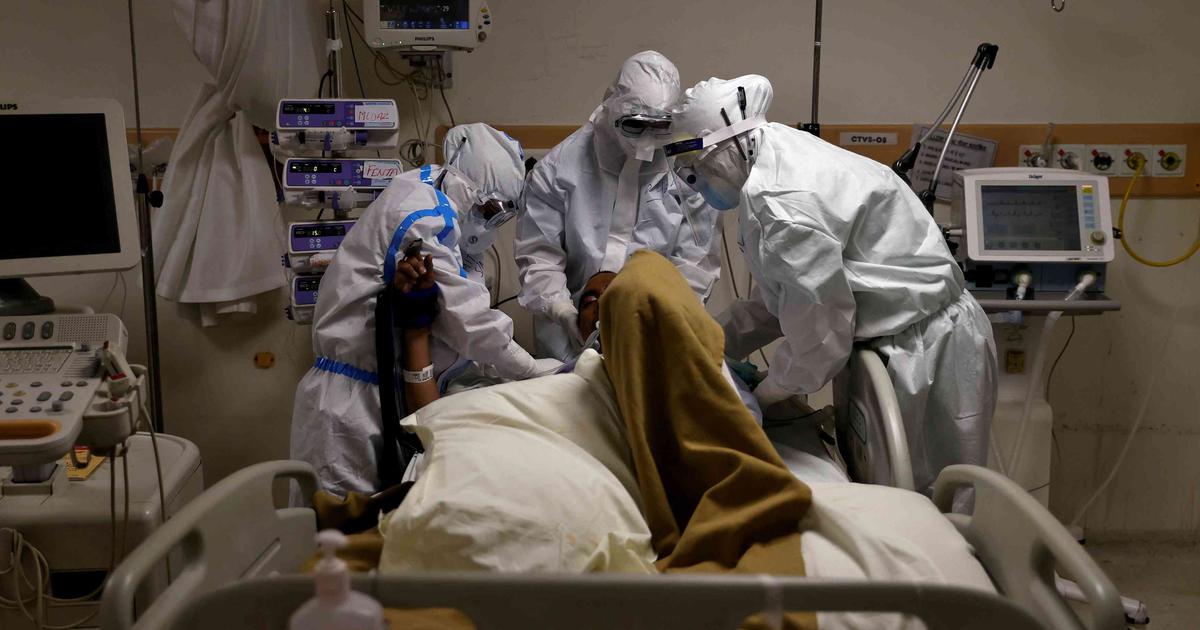
I chose to work at a COVID centre, I was not assigned.
Most intermediate care centres act as specialised centres for the treatment of COVID-19 patients, and are separate from the main hospitals. At hospitals, COVID-19 patients are categorised according to three levels: the isolation ward is where the mild to moderate COVID-19 patients are treated; the High Dependency Unit (HDU) treats moderate to severe patients; and the serious cases — patients requiring ventilators due to severe breathing problems — are treated at the Intensive Care Unit (ICU).
“During the first wave, I never went home,” said a doctor who works at a COVID-19 intermediate care centre outside Colombo. “My mother is diabetic and I was afraid [of passing on the virus to her]. A lot of my friends shared the same sentiments. But now, things have spun out of control.”
“Despite all of this, I never regret that I chose this career. I actually chose to work with Covid patients. I was not assigned,” she said.
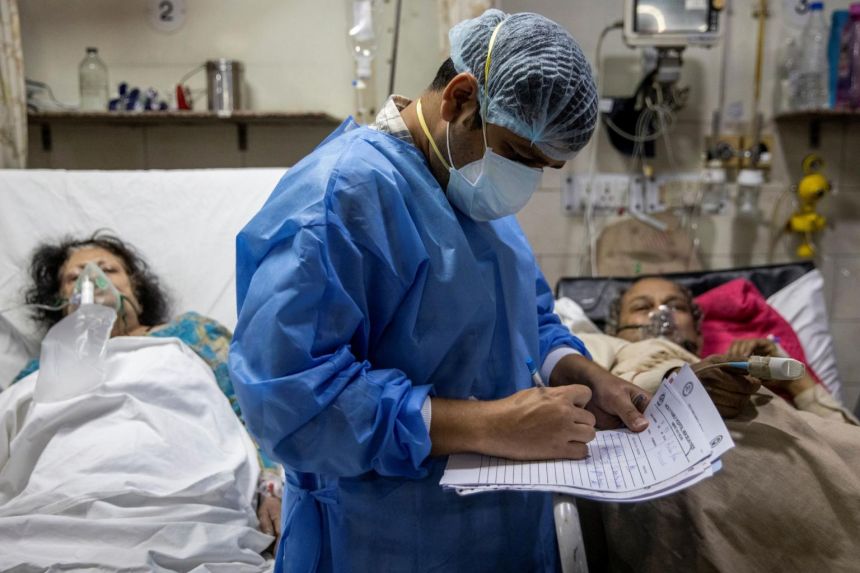
The doctor described how distraught both patients and caregivers are during the ongoing third wave. In comparison to the first and the second waves last year, the third, with its new COVID-19 variants, has brought with it an unforeseen severity; Sri Lanka has been recording more patients and more deaths.
“Some walk in healthy, but deteriorate without any warning,” the doctor said. “Some, we are able to save — others we cannot. [During] this wave, we have seen more deaths and admissions than the last two waves combined. There’s a death every day, and the sad part is [that] we are used to it.”
At the time of publication, Sri Lanka has officially recorded 2,581 COVID-19-related deaths. When the third wave was announced and nationwide travel restrictions imposed on 21 May, the death toll stood at 1,132. It took less than a month for that number to increase two-fold.
“We were massively understaffed at the beginning of May. It felt like the entire health system was collapsing,” the doctor said.
At that COVID-19 intermediate care centre, most patients are poor labourers or those from the fishing community. According to this doctor, patients range from beggars to small business owners. Many patients had not come with the intention of getting admitted; they had come seeking medication for a fever that they thought was normal, only to test positive for COVID-19, and be immediately sent to the unit managed by the doctor.
“The ones affected by COVID-19 are mostly the less fortunate… They are the ones who have to suddenly leave their families because they tested positive. Many do not have a place to quarantine,” the doctor said.
“There’s a very different scenario that happens within the walls of these hospitals, [compared to] what’s shown on TV or what’s seen on the road,” the doctor further explained.
We always fear that we will take the disease home with us
The case of the 60-year-old patient who was admitted with a severely infected leg wound is fresh in the memory of the surgeon at the base hospital. The patient had to undergo surgery multiple times, and was finally on the road to recovery, the surgeon recalled.
“He then contracted COVID when he was in the ward,” the doctor said. “We think it was probably from another patient or from someone who visited him. He didn’t recover.”
This has been a common occurrence during the third wave, according to the surgeon. There had been multiple cases of COVID-19 patients who had either contracted the disease or developed symptoms after they were admitted for a different cause.
Most patients, the doctor said, cooperate with the doctors and nurses. But many others, attached to various medical equipment (oxygen masks, CPAP masks, and machines), showed signs of depression.
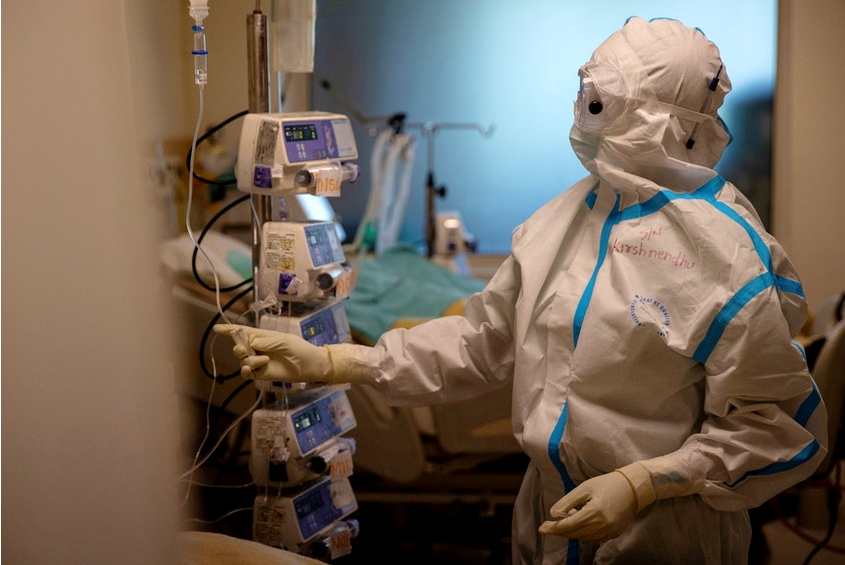
“My job, I wouldn’t say it’s difficult… [but] sometimes, it becomes very hard to operate on COVID patients when we are wearing protective gear. It limits our visibility a lot,” the doctor said.
He also spoke about how he witnessed many patients, young and not expected to be hard hit by the virus, develop a condition known as “long COVID” or post-acute COVID-19 syndrome.
“Patients [even after they recover from the disease] develop symptoms like fatigue, shortness of breath, and an inability to concentrate. But no one is talking about these conditions,” the doctor said. These complications can last weeks or months after the infection has gone away, the doctor explained.
Despite many of the frontline workers, such as this surgeon, and their immediate family members having received a vaccine against COVID-19, the anxieties of contracting the disease remain. “We are always in fear that we will take the disease home with us. Vaccination helps ease that burden, but not a 100 percent.”
I can’t see myself doing anything else
The 26-year-old doctor at a neonatal intensive care ward spoke about the experience treating babies who have tested positive for COVID-19: “It’s a difficult situation. When we do a rapid antigen test on the baby, it starts crying. And that would distress the mother and she would start crying. So we need to comfort the mother, do the rapid test on her baby, and then do another test on the mother as well,” the doctor said.
On 27 May, health authorities recorded the youngest COVID-19 fatality. He was only eight days old. The doctor was “lucky” not to have delivered a baby who developed severe symptoms of the disease. Beyond a fever, the babies the doctor had delivered who tested positive for COVID-19 “were not very ill or in a bad condition overall, thankfully.”
Special newborn intensive care is required for babies who become critically ill with COVID-19. However, such facilities are not widely available in Sri Lanka. Therefore, babies diagnosed with COVID-19 are transferred to hospitals in Colombo such as the Neville Fernando Teaching Hospital, along with their mothers.
“COVID or not, this profession is a difficult one. Regardless of the risk we put ourselves in every day — because of the number of patients we meet, not knowing if any of them are positive or not — we still do it day in and day out,” the doctor said, adding, “And I can’t see myself doing anything else other than working in the healthcare sector.